A 2026 study found that low β-hCG levels (≤50 mIU/mL at 9 days after blastocyst transfer) were linked to much lower live birth rates, and that how hCG rises over time is more predictive of outcome than the initial value.
β-hCG is one of the earliest measurable signs that embryo implantation has started, and most clinics rely on a single beta test about 9–12 days after transfer to confirm pregnancy.
Lower β-hCG levels are generally linked to worse outcomes, but it’s less clear how low is too low, especially when measured earlier than usual.
To investigate this, DiMarco et al. (2026) looked at IVF pregnancies with low initial β-hCG levels (≤ 50 mIU/mL) measured 14 days after fertilization (equivalent to 9 days after a blastocyst transfer, or 9dp5dt), and examined how often they resulted in live birth.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Study details
- Study type: Retrospective study conducted between 2019 and 2022 at a single fertility center in Canada
- Participants: 2,443 IVF pregnancies with a positive β-hCG after embryo transfer (median age 34)
- Low β-hCG group: 491 pregnancies with an initial β-hCG ≤50 mIU/mL
- Embryo stage: Mostly frozen blastocyst transfers, with 3.6% day 3 transfers
- Timing: β-hCG measured 14 days after fertilization (equivalent to 9dp5dt for blastocyst transfers)
- Statistical adjustment: Adjusted for age, BMI, stage of transfer, PGT-A use, number of embryos transferred
Lower live birth with low initial β-hCG
In this study, they used a cut-off of β-hCG 50 mIU/mL at 9dp5dt.
Live birth was lower when β-hCG was ≤50 mIU/mL (12% vs 57.8%), while biochemical pregnancy loss was much higher (65.2% vs 8.4%), with similar rates of clinical pregnancy loss between groups (14.3% vs 12.9%)
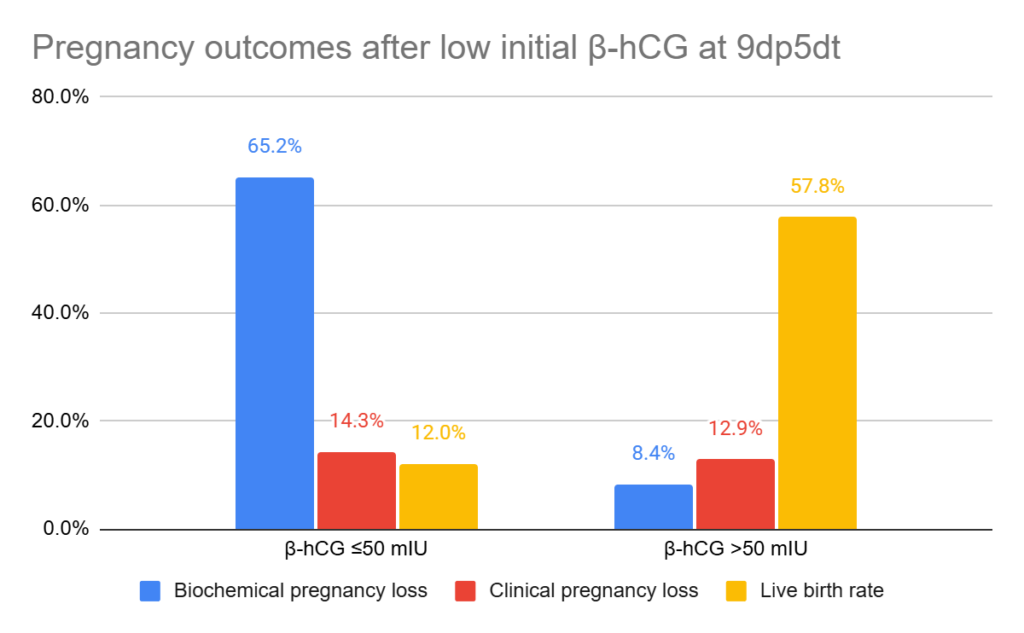
They found that each 10 mIU/mL increase in β-hCG was associated with a 4% increase in the odds of live birth (aOR 1.04 [1.03–1.04]).
The researchers did a separate analysis to identify thresholds linked to live birth:
- An initial β-hCG above 22.5 mIU/mL captured over 99% of live births, meaning live birth was very unlikely below this level, but it was still possible (the lowest β-hCG that resulted in a live birth was 6 mIU/mL)
- A level of 100.5 mIU/mL best separated outcomes at 9dp5dt, with about 66.4% of patients above this level having a live birth
The rise in β-hCG was more important than the starting value
In a separate analysis, the researchers looked at how β-hCG changed over time. Among pregnancies with low initial β-hCG (≤50 mIU/mL), how fast hCG increased was a better predictor of live birth than the starting number.
They found that a daily rise of about 44% was an important threshold for patients with low initial β-hCG. If the β-hCG didn’t rise this much, 99% of those pregnancies didn’t result in a live birth.
This was less predictive in pregnancies with higher initial β-hCG levels, where about 70% of pregnancies without a similar rise didn’t result in live birth.
There were also no live births when β-hCG levels declined.
Conclusion
This study showed that ≤50 mIU/mL initial β-hCG levels at 9dp5dt had a low chance of live birth and a higher risk of biochemical pregnancy loss. Levels below 22.5 mIU/mL were rarely associated with live birth, while higher values were linked to better outcomes.
Among pregnancies with low initial β-hCG, how the level changed over time mattered more than the starting number. A stronger rise was linked to better outcomes, while a slow rise or decline was almost always associated with a non-viable pregnancy.
Overall, this suggests that very low values (especially <22.5 mIU/mL) are rarely viable, but above that, outcomes depend more on how the hormone rises over time.
Want to read more about β-hCG levels and pregnancy?
Researchers in a 2019 study compared pregnancy outcomes with different serum β-hCG levels that were measured on day 16 of the embryo's age (13dp3dt/11dp5dt). Read more.
Researchers in a 2022 study found that women with low β-hCG (<149 mUI/ml) are more likely to have a preterm delivery and abnormal placental pathologies compared to women with higher β-hCG. Read more.
Researchers in a 2023 study developed a model to predict the chance of live birth after a positive β-hCG (beta-hCG), using the first measurement and a second one taken 48 hours later. Read more.
A small 2025 study found that most pregnancies show detectable hCG by day 6 after a blastocyst transfer, and those that first become positive on day 8–10 have higher rates of biochemical and ectopic pregnancy and a lower chance of ongoing pregnancy. Read more.
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.





