Diagnosed with premature ovarian failure and endometriosis, this patient went through 10 IVF cycles using her own eggs before finding success with a donor egg embryo. Her son was born in November 2022.
⚠️ These stories are personal experiences, not medical advice or scientific evidence. Success stories are more likely to be shared than unsuccessful ones, so they should not be interpreted as proof that a treatment works. Always discuss treatment decisions with your doctor.
✍️ Have a story to share? Submit your story.
📊 Story Snapshot
👩 Age: 44 at successful donor FET📆 Years trying: Over 6 years
🧬 Embryo: 5AA (donor egg)
🧪 Retrievals: 10 with own eggs, 1 with donor
🐣 Transfers: 6
💊 Diagnosis: Low AMH/DOR, Poor ovarian response, Endometriosis, Adenomyosis, Recurrent implantation failure (RIF), Immune-related issues
📈 Outcome: Live birth
I delayed IVF for years because of a severe needle phobia. At 34, I began working with a psychologist to try to overcome it, thinking I had time and not expecting any real issues. As a single woman, I was labeled “socially infertile,” but I had always been healthy, and my cycles were regular. Still, when I began fertility testing, the results were a blow: low AMH, high FSH, and an antral follicle count of just 5. I was diagnosed with premature ovarian failure.
At 39, I finally saw a fertility specialist. By then, my AMH had dropped to 3.7. I started taking supplements including Elevit, ubiquinol, and melatonin, and tried to optimize what I could. But by 41, my AMH was 2.6 and FSH was 35. At 42, my AMH had plummeted to 0.3. Despite it all, I pressed forward with IVF.
Over the next few years, I would go through ten IVF cycles using my own eggs. Most were canceled due to poor response. A few led to egg collections, but only one or two eggs at a time, and fertilization often failed. Cycle after cycle, I added new supplements and tried new protocols including DHEA, HGH, acupuncture, Chinese herbs, royal jelly, wheatgrass, estrogen priming, Saizen, Elonva, sildenafil pessaries, and dual triggers. I tried it all.
In 2019, I had a laparoscopy that revealed deep stage 3 endometriosis, which was surgically removed. I also had ovarian PRP around this time in hopes of improving my response. But even afterward, my cycles continued to fail. I had one faintly positive result, but my beta was too low and bleeding soon followed. Then COVID hit, and everything stopped.
When clinics reopened, I kept going. In one cycle, I developed six follicles and retrieved four eggs, but none fertilized. Another time, I ovulated just before retrieval. In total, I went through ten cycles. By the end, my FSH was 7, my best yet, but my estrogen didn’t rise and that cycle was canceled too. My clinic told me they would no longer approve further IVF using my own eggs.
That could have been the end of the story. But then someone following my journey on Instagram offered to donate their eggs. We met for coffee and immediately clicked. I moved forward with the donor cycle.
In March 2021, we retrieved eight eggs from one accessible ovary. Four embryos were created, and I transferred one. My beta was low but positive, 28 then 56, but I miscarried soon after. More heartbreak.
I wasn’t ready to give up. I had another laparoscopy in July and was also diagnosed with adenomyosis. My doctors prescribed Zoladex and later discovered I was homozygous for the MTHFR A1298C gene mutation. More endo was found in areas that had already been treated.
In November 2021, I got pregnant again, but the viability scan showed two empty sacs, and testing later revealed it had been a genetically normal boy. My fertility specialist now suspected immune rejection and prescribed immunosuppressants and vaginal probiotics for the next transfer.
In early 2022, I tried another transfer with a 5AA. I started with estrogen patches, sildenafil, and probiotics. My lining looked great, and we triggered for transfer. I used progesterone, immunosuppressants, aspirin, and Clexane.
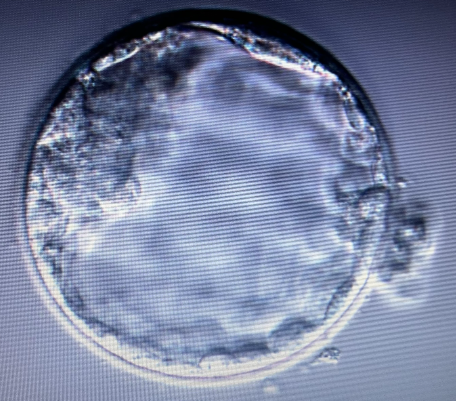
This time, the betas rose beautifully: 173, then 1187, then 3053, then 8950, then 18314, then 31165.
This embryo stuck.
The pregnancy wasn’t easy. I had hyperemesis, high blood pressure, gestational diabetes, and cholestasis. But none of it mattered. It was all worth it.
My son was born in November 2022. He turns 3 this year.
What would you say to someone who’s going through what you went through?
“Look into things yourself, ask lots of questions. Try not to compare yourself to other people too much – everyone is different.”
If you don’t feel you click with a specialist, change!
—@bigfatmisconception from Australia

Looking for more stories like this one?
You can explore similar IVF success stories by clicking the IVF Success tags below, browse the full archive here, or visit the Uterine Wall of Fame homepage.
Want to learn more about poor quality embryos? Check out my guide on poor quality embryo success rates.
✍️ Have a story to share? Submit your story.
