A 2026 meta-analysis examined how well PGT-A biopsies represented the rest of the embryo, and found higher mismatch rates in embryos labeled as aneuploid, especially segmental aneuploid embryos.
PGT-A works by removing a few trophectoderm cells from the blastocyst, and using those cells to estimate the chromosomal status of the embryo. While euploid embryos are usually prioritized for transfer, there have been reports of healthy births after transfer of embryos labeled as aneuploid, especially segmental aneuploids. This suggests that some embryos may be misclassified, resulting in potential false positive PGT-A results.
Jiang et al. (2026) combined the results of 22 studies in a meta-analysis to see how often embryo biopsy results disagreed with rebiopsies of the inner cell mass (ICM) or whole blastocyst, and whether certain types of PGT-A results were more prone to misdiagnosis.
In this study, the researchers reported these disagreements as “discordance,” but for simplicity I’ll refer to them as mismatch rates between the biopsy and the rest of the embryo.
For more background reading, check my Complete guide to PGT-A.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
What kind of PGT-A accuracy is this study looking at?
PGT-A companies often report very high accuracy rates. For example, CooperGenomics states that “many PGT-A tests are typically greater than 97% accurate” and references a 2020 study by Friedenthal et al. to support this claim.
However, that study mainly looked at pregnancies after transfer of embryos already classified as euploid. Specifically, it measured how often the genetics of a pregnancy, miscarriage tissue, or live birth matched the original euploid biopsy result. As pointed out by Paulson (2020), this creates an important selection bias, because embryos labeled as aneuploid are usually discarded and therefore are not included in these types of accuracy estimates.
This meta-analysis is looking at something different. Instead of following pregnancies after transfer, it examines how well the original embryo biopsy matches the ICM or the rest of the embryo itself after rebiopsy.
Study details
- Study design: Systematic review and meta-analysis of 22 studies published between 2000 and 2024.
- Participants: Studies included both euploid and aneuploid blastocysts from PGT-A and PGT-SR cycles.
- Location: Studies were mainly from China, the US, Japan, the UK, Belgium, the Netherlands, Canada and several other countries.
- DNA sequencing method: All studies used next-generation sequencing (NGS).
How often did PGT-A biopsies mismatch the embryo?
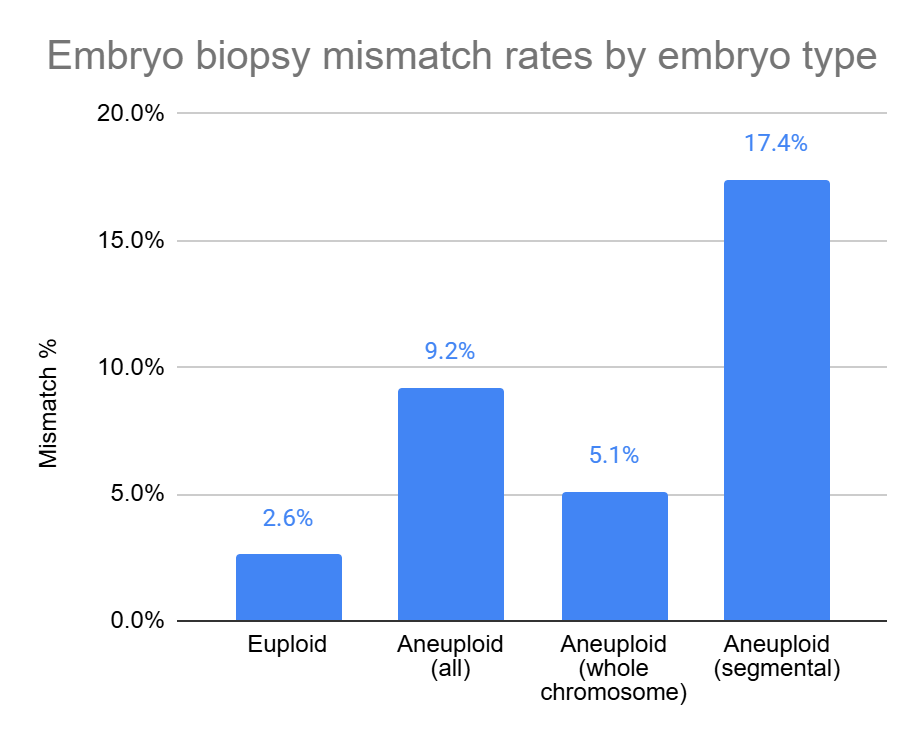
The researchers found that embryos labeled as aneuploid, especially segmental aneuploids, had higher mismatch rates than euploid embryos:
- Euploid embryos: 2.6% mismatch rate
-
All aneuploid embryos: 9.2% mismatch rate
- Whole chromosome aneuploid embryos: 5.1% mismatch rate
- Segmental aneuploid embryos: 17.4% mismatch rate
This means that nearly 1 in 5 embryos labeled as segmental aneuploid had a biopsy result that didn’t match the rest of the embryo.
The researchers also calculated odds ratios to compare mismatch rates between embryo types. Segmental aneuploid embryos showed the largest differences compared to euploid embryos.
- All aneuploid vs euploid embryos: Odds ratio [95% CI]: 2.82 [1.59–4.99], 15 studies, 1622 embryos, I2= 24.2%. This means that embryos labeled as aneuploid had 2.8-times higher odds of mismatch compared to euploid embryos.
- Whole chromosome aneuploid vs euploid embryos: 1.94 [1.08–3.50], 15 studies, 1246 embryos, I2= 7.1%.
- Segmental aneuploid vs euploid embryos: 9.31 [6.20–13.98], 12 studies, 793 embryos, I2= 0.0%.
- Segmental vs whole chromosome aneuploid embryos: 6.26 [2.57–15.22], 13 studies, 687 embryos, I2= 28.3%.
The authors also compared mismatch rates between embryos with a single chromosomal abnormality and those with multiple abnormalities, and found no significant difference. In other words, having more than one abnormal chromosome didn’t appear to increase the chance of mismatch for either whole chromosome or segmental aneuploid embryos. The study didn’t specify whether chaotic embryos with 6 or more abnormalities were included in this analysis.
Conclusion
This meta-analysis found that embryos labeled as aneuploid had higher mismatch rates than euploid embryos, with the highest rates seen in segmental aneuploid embryos. This shows that segmental aneuploid results may be more prone to misclassification.
The authors suggest that segmental aneuploid results should be interpreted more cautiously, and that embryos with this classification shouldn’t automatically be excluded based on a single biopsy result alone. They also note that repeat embryo biopsies may be considered in some cases to reassess the chromosomal status, although this involves additional embryo manipulation and potential risks.
There have now been several reports of healthy live births after transfer of embryos labeled as segmental aneuploid. Based on the limited data available so far, segmental aneuploid embryos appear to have ongoing pregnancy/live birth rates of around 24–31%. This is much higher than what’s been reported so far with whole chromosome aneuploids, with a live birth rate of about 1%.
These differences in live birth rates may be related to the mismatch rates shown in this study. The authors suggest that segmental abnormalities may be harder for current PGT-A methods to classify accurately because they involve smaller and more complex chromosomal changes than whole chromosome abnormalities. Since these smaller signals can sit closer to the limits of what the testing platform can reliably detect, technical noise or interpretation errors might sometimes cause an embryo to be incorrectly labeled as segmental aneuploid. This is likely less common with whole chromosome aneuploids because the chromosomal signal is much larger and easier for the testing platform to detect consistently.
Another possible explanation is sampling error. Since only about 5–10 cells from a blastocyst made up of hundreds of cells are biopsied, the sample may not always fully represent the rest of the embryo.
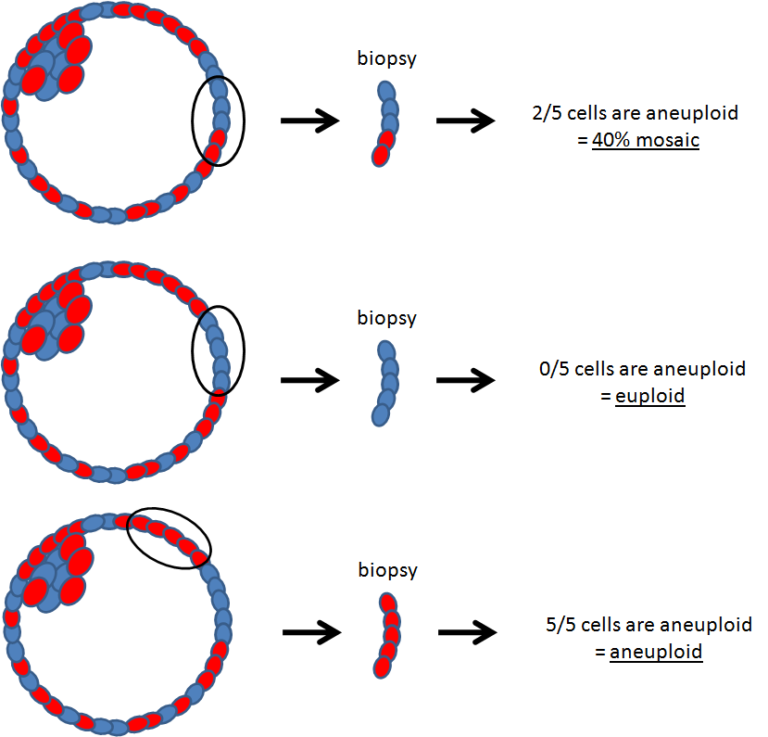
This study didn’t look at mismatch rates for mosaic embryos, although these are expected to be higher since mosaic embryos, by definition, contain a mix of normal and abnormal cells.
Limitations of this study include that most studies were retrospective and performed at single centers, laboratory and biopsy methods varied across studies, and some subgroup analyses included relatively small numbers of embryos. In addition, the study focused on mismatch rates between biopsies and embryo tissue rather than actual live birth outcomes after transfer.
Want to learn more about PGT-A accuracy and aneuploid embryos?
Evidence up to 2022 shows that a single PGT-A biopsy is highly concordant (similar) with the rest of the embryo when the embryo is aneuploid or euploid, but not when it’s mosaic or segmental. Read more.
Researchers in 2024 report on live births after segmental aneuploid transfers, finding that they have similar rates as high level mosaic segmental aneuploids. Read more.
Aneuploid embryo success rates after transfer are very low, with about 1–2% leading to a live birth, likely due to undetected mosaicism after PGT-A rather than true whole chromosome aneuploidy. Read more.
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.




