Researchers in 2021 developed a tool to predict the number of blastocysts formed based on IVF outcomes and clinical characteristics for women with different diagnoses.
Check out my complete guide to embryo grading and success rates to learn more about embryo development, grading and success rates.
Factors that influence how many day 3 embryos make it to blastocyst
One important factor that determines how many day 3 embryos make it to blastocyst is embryo quality on day 3. Day 3 embryos are evaluated on the basis of their cell number (with around 8 or more being ideal) and fragmentation (<10% is ideal). If you’re not clear on this, read my post on embryo grading and success rates.
One study (Sasikala et al. 2015) found that women who have <3 day 3 embryos and >3 day 3 embryos form blasts at the same rate – provided the day 3 embryos are good quality. Crosby et al. (2013) found that blastulation rates depend on the number of good quality day 3 embryos. Women with <3 good quality embryos had 43.1% of their day 3 embryos become blastocysts, while women with 4 or 5 had a higher blastulation rate (48.2% and 62.6% respectively).
Alikani et al. (2000) found that the highest rate of blastulation was in day 3 embryos with 7-9 cells and <15% fragmentation (~35%-40%). This was reduced to <10% blastulation with <5 cells, or about 10% with >25% fragmentation.
Another factor in predicting how many day 3 embryos make it to blastocyst is age. Vega et al. (2014) found a reduction in blastulation rates in women >35 years old compared to women <35 years old. They also found that day 3 embryos were more likely to become blastocysts if they were euploid (76.3% of day 3 euploids became blasts vs 25.5% of aneuploids).
A recent study by Jin et al. (2021) took it a bit further and found associations with diagnosis, female age, serum AMH, the number of oocytes retrieved, fertilization rate, and the rate of top-quality embryos on day 3. That’s a lot! They actually developed a special tool called a “nomogram” to help predict how many day 3 embryos make it to blastocyst using the above criteria.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Using a nomogram to predict blastulation rate
In the Jin et al. (2021) study, they compared blastulation rates and other characteristics for IVF cycles in women with tubal factor infertility, PCOS, and endometriosis. They used some fancy statistics (multivariable logistic regression) to test the association between blastulation rate and these characteristics.
They found that female age, AMH levels, the number of oocytes retrieved, the fertilization rate, and the top day 3 embryo rate were significantly associated with blastuation rate. So they assembled nomograms using this data to predict the blastulation rate from these characteristics for these three diagnoses.
Have a diagnosis besides PCOS or endometriosis? Use the tubal infertility one – this is based on the largest data set and these women generally had no egg quality issues. Not ideal but it’s the best of the three in this case!
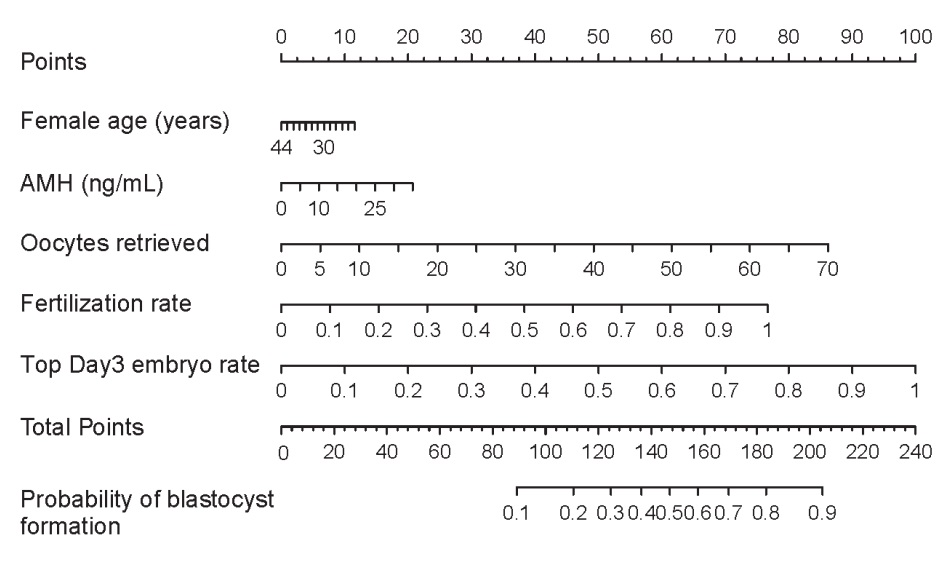
A nomogram is kind of like a calculator and can be used to do complex mathematical formulas. Kind of like how an abacus can be used as a calculator. Let’s first look at the nomogram for tubal factor infertility.

So to use this, you need to add up the points for each characteristic (female age, AMH, oocytes retrieved, etc.). Each characteristic has a line with different values that corresponds to a certain amount of points that you can see on top. As an example:
- 20 years old
- AMH of 5 ng/mL (go here to convert pmol)
- 20 oocytes retrieved
- 90% of mature eggs were fertilized
- 90% of fertilized eggs went on to produce top quality day 3 embryos (<10% fragmentation, 6-10 cells). Again, check my post on embryo grading and success rates to see how to evaluate this if you don’t know.
Drawing a line from each characteristic gives us a certain number of points. When you add up the points you can then draw a line toward the bottom to see the blastulation rate.

In this example, the blastulation rate is 0.82 or 82%. So about 82% of all day 3 embryos are predicted to become blasts based on this model.
Here is the nomogram for the PCOS diagnosis:
And the nomogram for the endometriosis diagnosis:

A few points to consider about the nomograms:
- This is a model based from a specific set of data, so it will not apply to everyone! In fact, they found it to exhibit “fair performance” when testing it (~75-80% accurate).
- Male factor was not assessed here because it can lead to lower blastulation. For this reason, ICSI cycles were not included (it’s okay if you used ICSI, but not if you used it because of male factor – they would need a new nomogram for that).
- The PCOS group had some issues, mainly they were generally younger and had a high AMH. So this might skew the results favorably for this nomogram.
- This data was based from a single center. Ideally, it needs to be validated using other centers.
- This is a retrospective study. Embryos that were used for these models were excess embryos after day 3 fresh transfers or freezing (my understanding is that the best 1-2 were used and the rest were taken to day 5 but this isn’t clear). Ideally, all fertilized eggs would be cultured to blast and then the models would be created.
Hopefully in the future these shortcomings are resolved. But for now, this is a pretty good way to predict how many day 3 embryos will become blastocyst – certainly better than the “30-50%” I’ve been using!
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.









