A 2025 study found that after a first frozen embryo transfer, experiencing an early pregnancy loss did not increase the risk of loss in the next transfer, for both euploid or untested embryos.
After a pregnancy loss from an embryo transfer, many patients and doctors worry that it signals an underlying problem that will repeat in future transfers.
A study by Barrett et al. (2025) examined whether experiencing a biochemical or clinical pregnancy loss after a first single frozen embryo transfer increased the risk of pregnancy loss in the next transfer, in both PGT-A tested and untested cycles.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Study details
- Study type: Retrospective study that took place at a US-based fertility center between 2017–2021.
-
Participants: A total of 2,385 patients (median age 35.2) who had their first and second consecutive single frozen embryo transfer:
- 2,103 patients had euploid–euploid FET pairs
- 282 had untested–untested FET pairs.
- Donor gametes, gestational carriers, ectopic pregnancies, terminations, and stillbirths were excluded.
- Since this study focused on first and second consecutive FETs, it was not designed to evaluate patients with established recurrent pregnancy loss or recurrent implantation failure. Information on pregnancy losses before IVF, from unassisted conception, was not available.
- Embryos: Single blastocyst frozen embryo transfers only. Most were day 5 or 6 and had A or B grades (about 10% were C graded).
- Primary outcome: Pregnancy loss (biochemical or clinical) after the second frozen embryo transfer.
Most patients proceeded to their second FET without major changes. The same endometrial preparation protocol was used in about 75-80% of cycles, additional treatments were not routinely added, and the second transfer was usually done within a few months, suggesting this was a straightforward next attempt.
No increased risk of second failed transfer after a first (euploid transfers)
In patients having a euploid frozen embryo transfer, researchers examined whether the outcome of the first transfer (implantation failure, biochemical pregnancy loss, or clinical pregnancy loss) affected outcomes in the second transfer. You can see the results of the second transfer below:
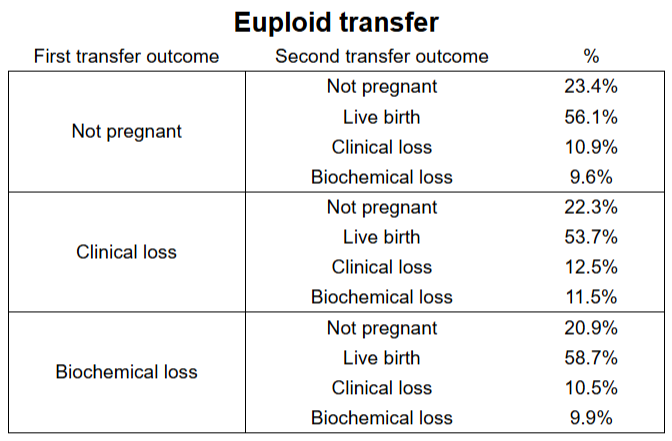
No matter what the result of the first transfer was, outcomes in the second transfer were consistent:
- No change in live birth rates — they ranged from 53.7% to 58.7%, regardless of whether the first transfer resulted in no pregnancy or a loss (p= 0.286).
- No change in rates for no pregnancy — they ranged from 20.9% to 23.4% (p= 0.554)
- No difference in clinical loss rates — they ranged from 10.5% to 12.5% (p= 0.42)
- No difference in biochemical loss rates — they ranged from 9.6% to 11.5% (p= 0.49)
This shows that a previous biochemical or clinical loss didn’t increase the risk of loss in the next euploid transfer, and that most patients had a live birth. An additional statistical analysis (regression), that controlled for female age, embryo quality, etc. showed no changes. In other words, with euploid embryos, a loss in the first transfer doesn’t “carry over” to the next one.
No increased risk of second failed transfer after a first (untested embryo transfers)
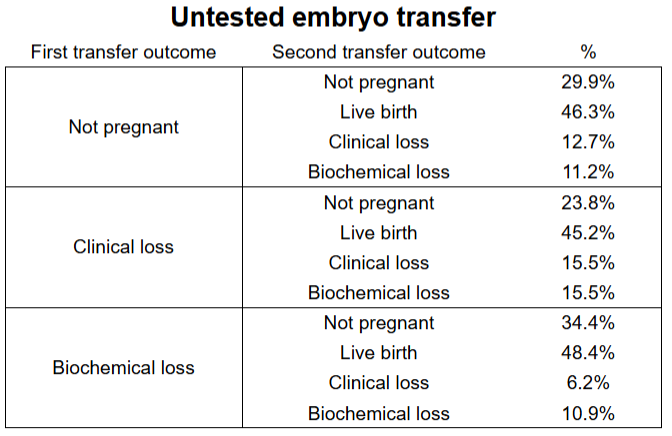

Like the euploid results, outcomes for untested embryos in a second transfer were consistent. A previous biochemical or clinical loss didn’t increase the risk of a loss in the next transfer.
- No change in live birth rates (p= 0.927)
- No change in rates for no pregnancy (p= 0.356)
- No change in clinical loss rates (p= 0.21)
- No change in biochemical loss rates (p= 0.582)
Conclusion
This study found that the outcome of a first FET didn’t affect the chances of success in the next transfer, whether it resulted in no pregnancy, a biochemical pregnancy, or an early miscarriage. Most patients had a live birth in their second FET, and there were no meaningful differences in rates of no pregnancy or pregnancy loss.
This pattern was seen for both euploid and untested embryo transfers.
Not all studies agree with this one. Some found better outcomes after a prior loss, others found no effect, and some suggested higher loss rates in later cycles. These studies also differed in embryo stage, transfer timing, and overall success rates, and none included PGT-A, which limits how well their findings apply to modern frozen embryo transfer cycles, the authors write.
Overall, the results suggest that an early loss after a first FET doesn’t “carry over” to the next attempt.
It’s important to note that this study followed patients going from their first to second frozen embryo transfer and was not designed to evaluate recurrent pregnancy loss or recurrent implantation failure. Pregnancy loss history from unassisted conception before IVF was not available, so some patients may have had prior losses.
Want to read more about pregnancy loss?
This post covers the variety of reasons embryos can fail to implant or miscarry, including as a result of advanced maternal age, chromosomal translocations, lifestyle, endometritis, the microbiota, immunological issues, endometrial receptivity, the clinic, and more. Note that this is not a complete list, and will be updated periodically. Read more.
A 2025 study suggests that most patients with recurrent pregnancy loss who transfer up to 3 euploid embryos go on to have a live birth, though data from later transfers are limited. Read more.
Even when embryos are euploid and pass PGT-A, miscarriage can still happen. A new 2025 study suggests that genetic mutations too small to be seen by standard PGT-A may explain some of these losses. Read more.
A 2024 study found that patients with recurrent pregnancy loss have congenital uterine anomalies at a rate of 8-19%, with 23% having adenomyosis. Read more.
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.