Researchers in a 2023 study found that patients with or without endometriosis have comparable live birth rates after transferring a euploid embryo, although patients may have been surgically treated (a limitation). Endometriosis patients were more likely to produce aneuploid embryos.
This study compared outcomes after transferring a single euploid embryo in patients with or without endometriosis.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Study details
This section covers key details of how the study was performed, including the number of patients and their characteristics, how they were treated, and other methods used. For those who aren’t interested in these details, and just want to see the results, you can go ahead and skip this part.
- This was a retrospective cohort study that took place between 2015 and 2021 at a single IVF center in China.
- Patients did PGT mainly because they were carriers for affected chromosomes or mutations, or were of advanced maternal age.
- Endometriosis patients were surgically diagnosed with endometriosis. Not all of the control patients had laparoscopy to confirm the absence of endometriosis, which is a limitation.
- PGT-A was only performed on day 5/6 blastocysts with a grade greater than 4BC.
- Only a single PGT-A tested euploid was transferred.
- The paper doesn’t specifically mention the type of FET, although it seems to be a standard medicated procedure, with progesterone administration either orally or transvaginally.
- The paper does not specify whether patients in the endometriosis group received surgical treatment. However, in clinical practice, most patients undergoing laparoscopic diagnosis of endometriosis are treated during the same procedure, typically through excision or ablation of visible lesions.
In terms of sample size, there were 128 patients with endometriosis who had 174 frozen embryo transfers, and 497 patients without endometriosis who had 522 FETs.
In terms of baseline characteristics, the patients were about 32 years old and mostly had similar characteristics.
No difference in live birth rates and other clinical outcomes in patients with endometriosis
After transferring a single euploid, there was no difference in the live birth rate in patients with or without endometriosis (52.3% vs 57.3%, p= 0.252).
For endometriosis vs the control group, there was no difference in the clinical pregnancy rate, miscarriage rate or preterm birth rate (63.2% vs 67.4%, p= 0.308; 4.6% vs 6.5%, p= 0.358; 3.4% vs 4.8%, p= 0.458).
They also looked at patients who had a more advanced stage of endometriosis with endometriomas. These patients also didn’t show any differences to the control group after transferring a euploid.
Increased aneuploidy in patients with endometriosis
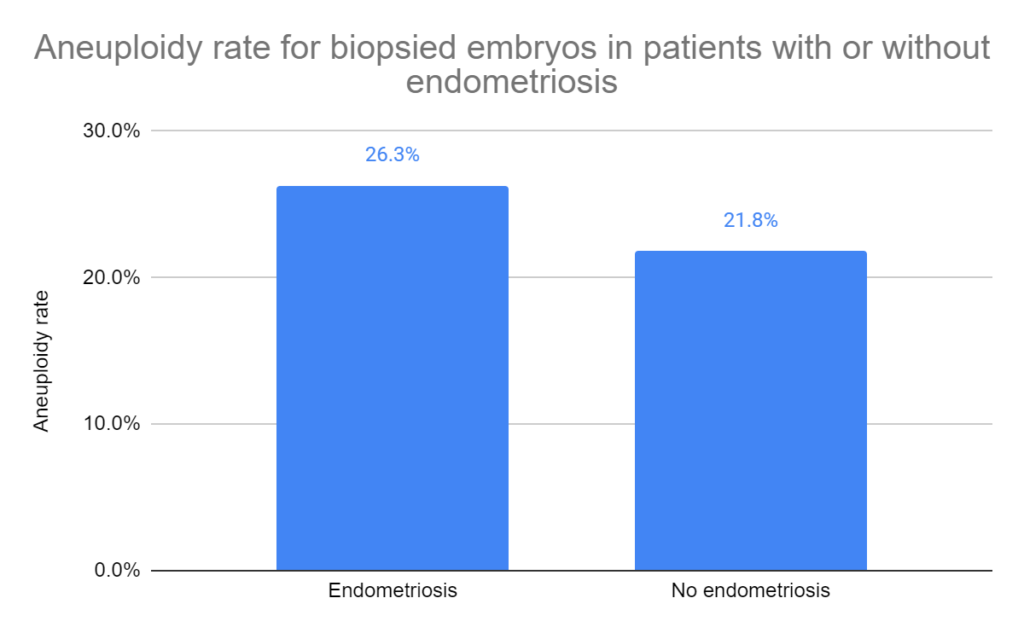
There were a total of 745 blastocysts biopsied from endometriosis patients and 2,195 from patients without endometriosis. They found an increased aneuploidy rate for patients with endometriosis (26.3% vs 21.8%, p= 0.012). Note that these appear to be very low aneuploid rates, but this may be because they biopsied better quality embryos in patients <35. You can check out typical euploid rates based on age here.
They also did an analysis on patients with different types of chromosomal abnormalities (inversions, balanced translocations, etc). They found that patients with a specific type of translocation, called a Roche translocation, were more likely to produce aneuploid embryos if they had endometriosis.
Conclusions
For patients with or without endometriosis who transferred a single PGT-A tested euploid, this study found no differences in live birth, clinical pregnancy, miscarriage or preterm delivery rates.
They did find that women with endometriosis were more likely to produce aneuploid embryos, indicating that there might be reduced egg quality in these patients. Despite this, the increase in aneuploidy was small, so it’s not clear if it’s clinically significant.
However, it wasn’t clear if patients diagnosed with laparoscopy also received surgical treatment, which is often the case.
There isn’t much research that compares aneuploidy rates in patients with endometriosis, so larger studies are needed.
A recent meta-analysis also found no difference in live birth rates and other clinical outcomes in patients with endometriosis, although the meta-analysis didn’t account for surgical or medical treatment of endometriosis.
There are some limitations to this study:
- They didn’t confirm that all their control patients were free of endometriosis by laparoscopy. The authors seem to be confident that the patients in the control group don’t have endometriosis, as they were seeking PGT for different diagnoses.
- The study could be expanded to include more patients.
- There was no mention of treatment of the endometriosis group.
- They didn’t indicate the embryo quality between the groups. Maybe the endometriosis patients were more likely to have poorer quality embryos, which resulted in an increase in aneuploidy.
Related studies
Not all research may agree with this study. There were a number of studies referenced that you might want to check out, as shown below (4 links):
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.










