Researchers in a 2023 study show that poor quality embryos have acceptable live birth rates compared to good and fair quality embryos, with only a slight increase in pregnancy loss and no differences in perinatal outcomes.
The quality of a blastocyst has been linked to IVF success rates, with lower quality embryos performing worse than higher quality embryos, leading many labs to discard them.
Zou et al. (2023) wanted to assess the pregnancy outcomes of poor quality embryos compared to good and fair quality embryos, while also looking at perinatal outcomes like birthweight and preterm births.
To better understand this post, you might want to check out my Complete guide to embryo grading and success rates, particularly the section on day 5 blastocyst grading.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Study details
- This was a retrospective study that took place between 2009 and 2020 across 14 IVF clinics in 3 countries.
- Only a single fresh or frozen blastocyst was transferred.
- Good quality blastocysts were AA, AB or BA; fair quality were BB; poor quality were AC, CA, BC, CB or CC.
- Only embryos with an expansion of 3 or higher were included (no early blastocysts).
This study involved 10,964 blastocyst transfers: 4,386 were good quality, 3,735 were fair quality and 2,843 were poor quality.
In terms of baseline characteristics, the average age was about 33, and there were differences between fresh/frozen transfers, the day the blastocyst was transferred, its expansion, its grade, etc. These were statistically adjusted in their analysis.
Pregnancy outcomes of good, fair and poor quality blastocysts
Compared to good quality blastocysts, both fair and poor quality blastocysts had lower clinical pregnancy and live birth rates, while pregnancy loss rates were higher.
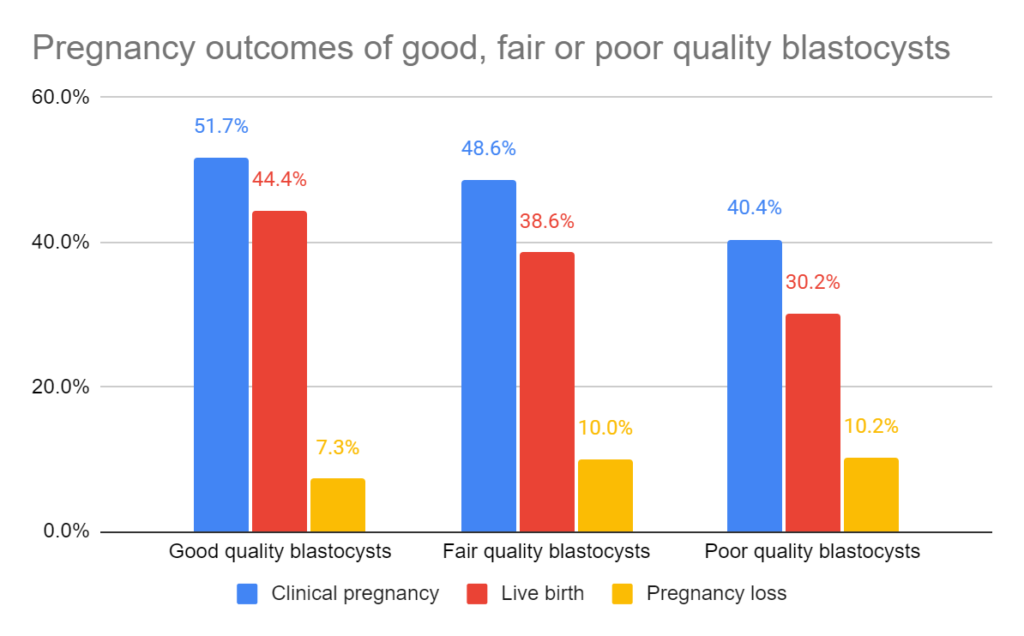
This was statistically significant for each outcome (for example, for the live birth rates, the adjusted odds ratio [95% CI] was 0.70 [0.62-0.77] for fair quality and 0.48 [0.41-0.55] for poor quality). This odds ratio of 0.48 means that, after statistical adjustment, the odds of live birth with poor quality embryos was about half that of good quality embryos.
They also reported on live birth stratified by age, as shown below.
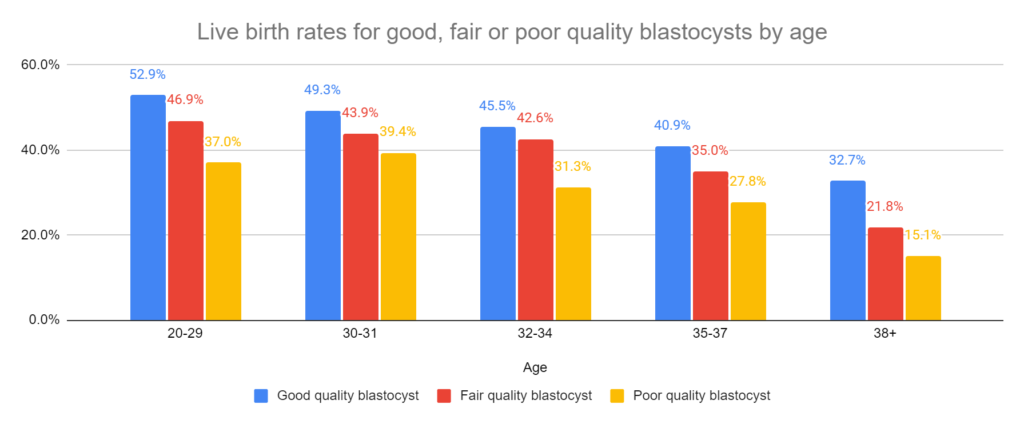
Poor quality embryos have acceptable pregnancy outcomes
They compared the different types of poor quality embryos (ie. AC, CA, BC, CB, CC) to good quality embryos. Live birth rates were highest when the poor quality embryo had an A quality ICM or trophectoderm, followed by embryos with a B, and lowest with a CC. This was all statistically significant (the adjusted odds ratios [95% CI] for BC, CB and CC were 0.53 [0.46-0.63], 0.35 [0.28-0.43] and 0.30 [0.18-0.52]).
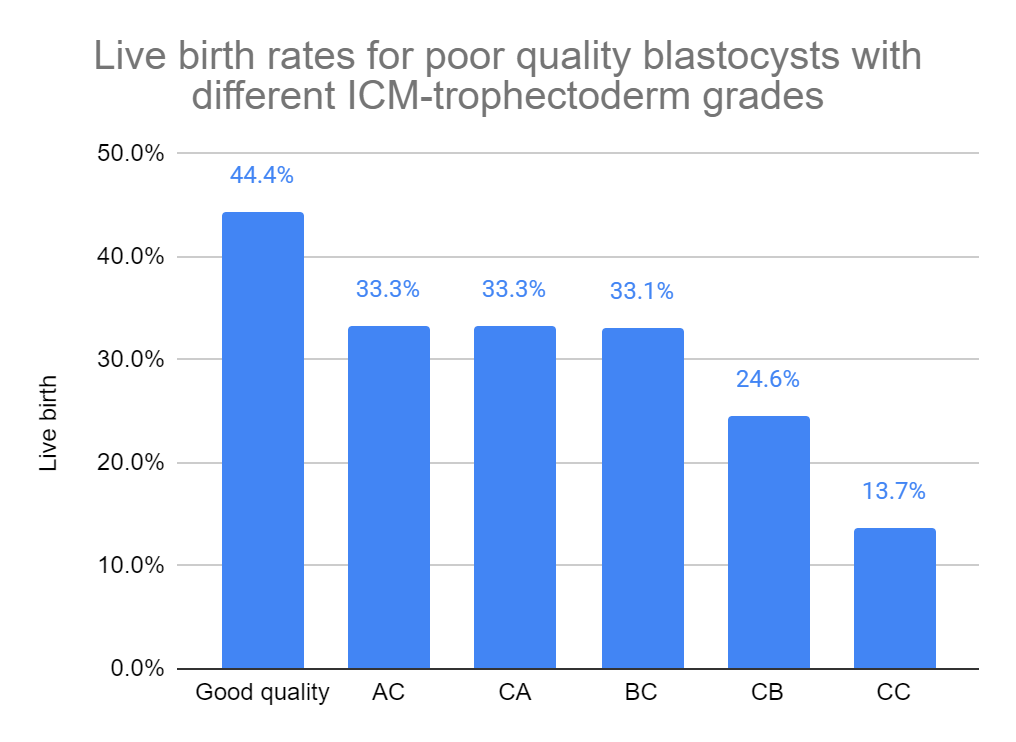
Pregnancy loss rates for BC and CB were higher compared to good quality embryos (10.8%, 10.5% vs 7.3%). The AC, CA and CC groups were smaller so there weren’t many clinical pregnancies to work with, but they didn’t find any differences from the good quality group.
They also did a comparison for day 5 and day 6 poor quality embryos. Miscarriage rates were similar, but live birth and clinical pregnancy rates were lower for day 6, which was statistically significant (adjusted odds ratio [95% CI]: 0.58 [0.48-0.70], 0.57 [0.47-0.68]).

No differences in perinatal outcomes across blastocyst qualities
They also looked at perinatal outcomes, and found no differences across the groups after statistical adjustment:
- Preterm birth
- Birthweight (very low/low/normal/high)
- Birthweight (small/appropriate/large for gestational age)
They also didn’t find any perinatal differences between poor quality day 5 or day 6 embryos.
Conclusions
This study found that poor, fair and good quality embryos all had different clinical pregnancy and live birth rates. The odds of a live birth using a poor quality embryo was about half that of a good quality embryo.
Pregnancy loss rates were higher with poor quality embryos, but not by much.
Live birth rates decreased with poor quality day 6 embryos compared to day 5, but was still acceptable.
As female age increased, the live birth rate dropped for each group. Poor quality embryos in women aged 20-29 had a higher chance of live birth compared to good quality embryos for women 38+.
In this study, any blastocyst with a C grade was considered poor quality. They found that AC, CA, BC and CB embryos had better live birth rates than CC embryos.
There were no differences in any of the groups in terms of preterm birth and birthweights.
This study shows that poor quality embryos have acceptable live birth rates that result in healthy babies. This research agrees with other studies that have been published, which I review in my post Grade C (poor quality) embryo success rates.
The authors state that CC blastocysts can still result in healthy babies, particularly when good quality embryos are limited or if there have been previous difficulties conceiving.
Related studies
Not all of the research on this topic may agree with this study. For those who are interested in learning more, here are links to 5 related studies that were referenced in the article:
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.










