This post explores how different popular diets can affect fertility and IVF outcomes, including the Mediterranean, DASH, vegetarian, keto and Western diet. Some diets can benefit metabolic health and fertility, particularly for PCOS patients, while others have a negative effect.
Lifestyle and diet can significantly impact fertility by affecting hormonal and physiological functions in the body. Getting the right nutrients is crucial for reproductive health, and could contribute to egg and sperm quality.
In this post we’ll cover some popular diets and how they can impact fertility and IVF outcomes.
For more information on egg quality and development, check out my Complete guide to egg quality. If you also want to learn more about sperm health, check out my Complete guide to sperm quality.
This post uses a recent review by Salvaleda-Mateu et al. (2024, CC BY 4.0) as a base, with additional references from other studies included.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Table of Contents
Mediterranean Diet

The Mediterranean diet is known for high consumption of olive oil, fruits, vegetables, nuts, cereals; moderate consumption of fish, meat, dairy and red wine; and low consumption of eggs and sweets. This diet has been linked to significant reductions in cardiovascular disease risk, diabetes, and certain cancers, primarily due to its ability to improve blood pressure, cholesterol levels and inflammation (Guasch-Ferré and Willett 2021).
The Mediterranean diet is considered the gold standard for diets due to its health benefits, and studies on infertility and diet sometimes use this diet as a control. Generally, studies on the Mediterranean diet in reproductive health show mixed results. Limited studies show improvements in sperm quality and reduced incidence of low birth weight, but clinical pregnancy and live birth rates results are inconsistent, with some studies showing benefits. There may be an increase in egg/embryo quality.
- Kermack et al. (2019) performed an RCT where patients adhered to a “Mediterranean diet” for 6 weeks before IVF (with increased omega-3 fatty acids, vitamin D and olive oil). There were no changes in blastocyst quality, but there were improvements in day 3 embryo quality (measured by KIDScore). They didn’t find any differences in clinical pregnancy or live birth rates. You can check out my summary of this study in my post Mediterranean diet and IVF – a clinical trial.
- Montano et al. (2021) performed an RCT involving a 16-week Mediterranean diet and physical activity intervention in healthy men, finding improved sperm concentration, motility and morphology.
- Crovetto et al. (2021) performed an RCT on pregnant patients following the Mediterranean diet and found a reduction in babies born with a low birth weight (14% vs 21.9%).
- Winter et al. (2023) and Muffone et al. (2023) conducted meta-analyses that showed conflicting results in clinical pregnancy and live birth rates with the Mediterranean diet. While Winter et al. (2023) found a benefit in clinical pregnancy live birth rates (1.91 times higher), Muffone et al. (2023) didn’t, although they did find an improvement in sperm concentration and count (about 2.5 times higher).
- Karayiannis et al. (2018) found that women with the highest adherence showed improved live birth rates compared to women with the lowest adherence (26.6% vs 48.8%). There were no differences in the number of eggs retrieved, fertilization rate or embryo quality.
- Sun et al. (2019) found that patients with high adherence to the Mediterranean diet had a larger number of embryos available (8.40 vs. 7.40), with no differences in clinical pregnancy rates.
DASH Diet
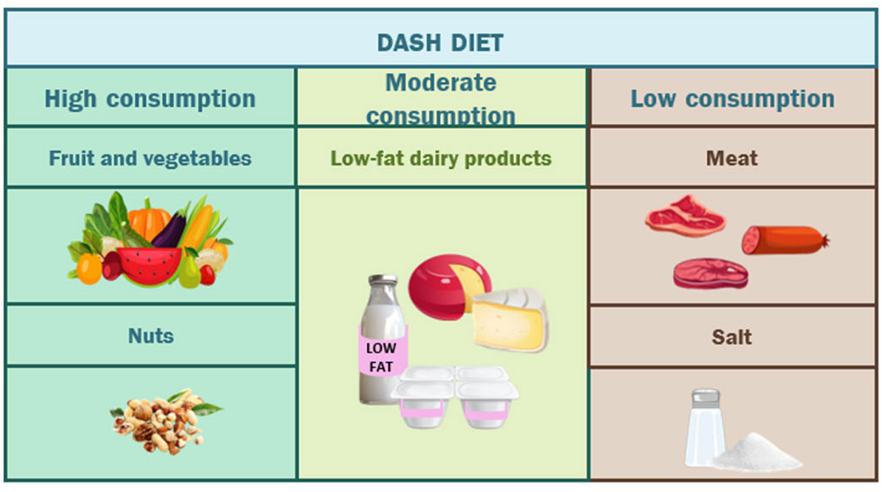
The Dietary Approaches to Stop Hypertension (DASH) diet is designed to help lower blood pressure and reduce the risk of hypertension. It’s high in fruit, vegetables and nuts, moderate in dairy and low in meat and salt. The DASH diet has a particular focus on the intake of nutrients that are known to help lower blood pressure, such as potassium, magnesium, and calcium, and it has strict guidelines for sodium intake. It’s been shown to have benefits in treating hypertension (Theodoridis et al. 2023).
Recent studies on the DASH diet in reproductive health have shown that it can improve insulin resistance, reduce abdominal fat, and enhance sperm quality, as well as improve BMI and metabolic profiles in patients with PCOS. However, limited evidence has shown no benefit in clinical pregnancy or live birth rates in patients undergoing IVF or IUI.
- Asemi and Esmaillzadeh (2015) performed an RCT on overweight/obese patients with PCOS, and found that the DASH diet improved insulin resistance and reduced abdominal fat.
- Foroozanfard et al. (2017) performed an RCT on women with PCOS and found improvements in BMI, AMH, insulin and metabolic profiles after 12 weeks on the DASH diet.
- Salas-Huetos et al. (2023) evaluated the DASH diet in patients undergoing IVF or IUI and found no benefit in clinical pregnancy or live birth rates.
- Danielewicz et al. (2019), Efrat et al. (2018) and Cutillas-Tolín et al. (2019) found that the DASH diet improved sperm quality, mainly by increasing sperm count and concentration. Salas-Huetos et al. (2023) didn’t find that DASH improved sperm quality.
Vegetarian and vegan Diets
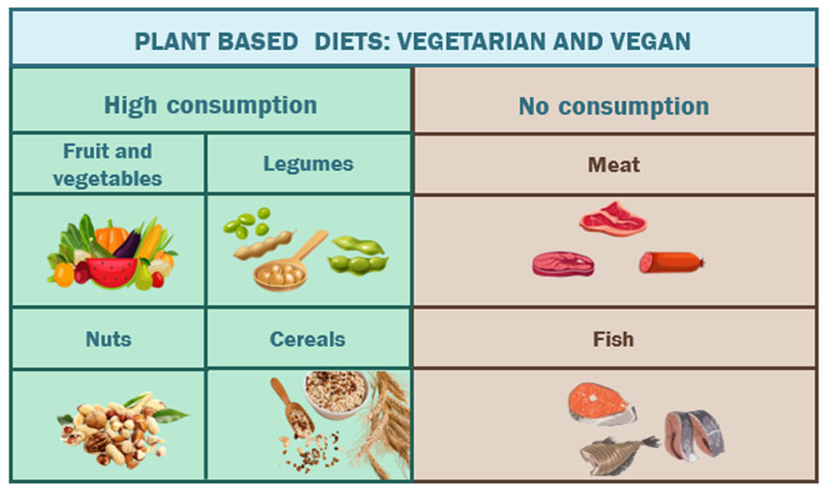
Vegetarian and vegan diets are high in vegetables, grains, nuts and fruits. Vegetarian diets exclude meat and seafood, while vegan diets further exclude all animal products, like dairy, eggs and honey. Vegetarian and vegan diets can reduce the risk of diseases like diabetes, heart disease and obesity, but if not carefully planned, they can lead to deficiencies in nutrients like vitamin B12, iron, zinc and calcium (Wang et al. 2023).
Research has shown mixed outcomes of vegetarian diets on reproductive health: they might be linked to menstrual disorders and lower birth weights, potentially due to inadequate nutrition. However, adherence to a healthy plant-based diet could shorten times to pregnancy. Studies found no significant differences in hormone levels and sperm quality between vegetarians and omnivores, but soy components in vegetarian diets could affect male fertility.
- Some studies have found an association with vegetarian diets and menstrual disorders, and in a review by Griffith and Omar 2003, the authors aren’t clear if this association is due to the diet itself or from inadequate nutrition.
- Lim et al. (2022) found that women with higher adherence to a healthy plant-based diet had shorter times to pregnancy compared to those following an unhealthy plant-based diet, which included high intake of fast food and sugary drinks.
- Samimisedeh et al. (2024) performed a meta-analysis that compared vegetarian and omnivore diets, and found no differences in sex hormone levels in women (7 studies), except for estrone (a type of estrogen) in vegetarians.
- Yisahak et al. (2021) found that vegetarians were at increased risk of giving birth to babies that were small for gestational age, possibly due to reduced weight gain during pregnancy. A meta-analysis by Tan et al. (2019) found that low birth weights were only statistically significant in Asian women following a vegetarian diet compared to omnivores.
- Vegetarian diets may be rich in soy-based foods, which contain isoflavones that can have estrogen-like effects and can lead to male fertility problems (West et al. 2005). Samimisedeh et al. (2024) performed a meta-analysis that compared vegetarian and omnivore diets, and found no differences in sperm quality (16 studies).
Ketogenic Diet

The ketogenic diet is high in fats and low in carbohydrates, leading the body into ketosis where fat is the main energy source. It can help manage conditions like obesity, epilepsy and type 2 diabetes by lowering insulin and glucose levels. However, it raises LDL cholesterol, which could increase cardiovascular risks, and long-term use might cause nutritional deficiencies and health issues like kidney stones and liver disease (O’Neill and Raggi 2020).
Recent studies show that a ketogenic diet significantly benefits obese/overweight women with PCOS, enhancing menstrual regularity, insulin resistance, and endometrial thickness, and reducing BMI, body circumference, and OHSS risks. However, there are potential concerns, such as negative impacts on fetal neurological development observed in animal studies.
- Pandurevic et al. (2023) performed an RCT and found significant improvements in spontaneous ovulation cycles in obese women with PCOS following a ketogenic diet for 8 weeks compared to a Mediterranean diet (38.5% vs 84.5%).
- Meneghini et al. (2023) observed that overweight/obese PCOS patients following a very-low-calorie keto diet for 120 days and experienced decreased BMI and body circumference, improved insulin resistance and menstrual regulation, increased AMH levels, higher AFC, and a lower risk of OHSS compared to those on the Mediterranean diet.
- Palafox-Gómez et al. (2023) found improvements in insulin resistance markers and endometrial thickness in patients with PCOS who followed the keto diet for 14 weeks, with no difference in the number of eggs retrieved or fertilization. These PCOS patients had a failed first IVF cycle, and after following the keto diet in their second cycle, 8 out of 12 had a live birth.
- Besides some of the risks mentioned above, animal experiments have shown that the keto diet may also have a negative effect on fetal neurological development (Rugiel et al. 2023, Barry et al. 2018).
- Animal studies (reviewed by Kulak and Polotsky 2013) have shown that shifting the energy source from glycolysis to ketosis is associated with an improvement in mitochondrial function, which might have benefits on fertility.
Western Diet

The Western diet is characterized by its high intake of red and processed meats, unhealthy snacks, sweet foods, sugary desserts and drinks, and ultra-processed foods (junk and fast food), along with low fruit and vegetable intake. The Western diet is essentially the opposite of the Mediterranean diet. This diet is linked to increased risks of obesity, diabetes, heart disease and cancer due to increased inflammation, poor gut health and lower antioxidant levels (Clemente-Suárez et al. 2023).
In terms of reproductive health, the Western diet has been linked to decreased sperm quality and increased asthenozoospermia. Additionally, studies in non-human primates suggest that this diet may induce inflammation in follicular fluid and reduce blastocyst formation during IVF.
- The widespread adoption of this diet has been linked to a global increase in obesity (Rakhra et al. 2020) and PCOS (Foley and Marsh 2019).
- Toledo et al. (2011) found that greater adherence to the Mediterranean diet was linked to a lower chance of experiencing difficulties in conceiving, which wasn’t seen with the Western diet.
- Multiple studies have linked the Western diet to reduced sperm quality, with a meta-analysis by Arab et al. (2017) showing reduced sperm concentration, but no effect on other semen parameters (6 studies). Some studies have found an increased risk of asthenozoospermia with adherence to the Western diet (Eslamian et al. 2012, Eslamian et al. 2014).
- Ravisankar et al. (2021) found that the Western diet led to inflammation in the follicular fluid of non-human primates, along with decreases in the number of blastocysts after IVF. Reduced blastocyst formation in non-human primates was found in another study from the same group (Ravisankar et al. 2022).
Conclusion
Here’s a brief summary of each of the covered diets and their impact on fertility:
- Mediterranean diet: Rich in olive oil, fruits, vegetables and nuts, it improves cardiovascular health and has shown mixed effects on sperm and embryo quality, with inconsistent effects on pregnancy and live birth rates.
- DASH diet: Aimed at lowering blood pressure, it features high fruit, vegetable and nut intake with low meat and salt, and has been shown to improve metabolic profiles in PCOS patients, but mixed results on pregnancy or live birth rates.
- Vegetarian and vegan diets: Excluding meat and possibly animal products, these diets reduce chronic disease risks but may cause nutrient deficiencies and have mixed effects on reproductive health, including potential low birth weights.
- Ketogenic Diet: High in fats and low in carbs, it helps with obesity and diabetes management and has shown significant benefits for PCOS patients, with potential cardiovascular risks.
- Western Diet: High in processed meats and sugary foods but low in fruits and vegetables, it is linked to higher obesity and disease rates and studies have shown negative effects on sperm quality and embryo development.
There are a number of limitations when it comes to dietary studies:
- Most are based on self-reported data, which is prone to errors and biases such as underreporting or overreporting food intake or recall inaccuracies
- Many dietary studies use observational study designs that can’t establish causality, meaning they can’t definitively prove that specific diets cause the results being measured.
- There could be individual differences in genetics, lifestyle factors (like physical activity), and use of medications. These confounders can give misleading results.
- Dietary studies often lack standardized meals, leading to inconsistencies in nutrient composition and portion sizes across different studies. There can also be cultural and geographic differences, and diets can change over time.
- Many studies use small sample sizes and are short-term.
While some of the studies here may not have these limitations, higher quality research is needed in general, with standardized diet interventions that are longer and include more patients. Additionally, more studies are needed to examine the impact of diet on IVF outcomes in infertility patients, including research on diverse patient groups that go beyond those with PCOS.
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.









