Researchers in a 2021 review combined multiple studies on assisted hatching and found no clear improvement in live birth rates, though clinical pregnancy rates were slightly higher and the chance of multiple pregnancy increased.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
What is the zona how does an embryo hatch?
The human egg is surrounded by a thick “shell” known as the zona pellucida (or zona for short). The zona doesn’t contain any cells, but is made up of glycoproteins, carbohydrates, and special proteins involved in binding sperm (including ZP1, ZP2, ZP3, and ZP4).
The zona is pretty useful!
- After fertilization it “blocks polyspermy” by hardening. This prevent multiple sperm from fertilizing the egg.
- It keeps all of the embryo’s cells held together (otherwise the embryo might fall apart).
Once the embryo develops into a blastocyst it begins to expand. Eventually, the blastocyst gets so large that it causes the zona to become thinner, until it eventually tears and the embryo can begin to hatch out.

Hatching is important because the cells of the trophectoderm need to attach to the cells of the endometrium in order to begin the implantation process.
What is assisted hatching?
Now that we’ve discussed the natural phenomenon of embryo hatching, let’s describe how an embryo can be “assisted hatched” in the IVF lab. Assisted hatching is where the zona is artificially disrupted and involves either thinning the zona by using chemical treatment, or by removing a small section of the zona entirely.
Assisted hatching can occur in a number of ways. A special acidic medium called Tyrode’s medium can be used to degrade the zona; a needle can be used to cut away a portion of the zona; or a laser can be used to introduce a tiny hole. Laser assisted hatching is the most commonly done as of 2021.
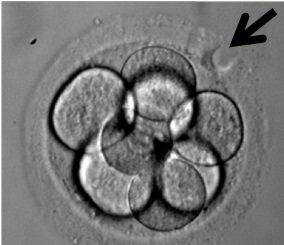
Why do we use assisted hatching?
Hatching is a process that needs to happen for the embryo to begin implanting. Once the embryo is transferred we can’t keep an eye on it anymore to make sure it’s hatching as it should be.
We know that in some cases, some eggs have thick zonas and this might have an impact on implantation rates (Loret de Mola et al. 1997). In addition, zona “hardening” after culturing, or freezing/thawing, has been suggested as a reason for assisted hatching. It’s not clear how, or even if this happens, although some studies have found physical changes in the zona after freezing that might affect the embryo’s ability to hatch (Valojerdi et al. 2010). These types of situations may be more common in older women, or those with higher basal FSH levels.
So assisted hatching is more of a fail safe to make sure the embryo can hatch – whether it’s a thickened zona, or the mysterious “zona hardening”, or some other phenomenon.
Does assisted hatching improve IVF success rates or outcomes?
The big question of course! There have been a lot of studies, so the best way to handle this is to look at a big review. A recent 2021 Cochrane review performed a meta-analysis on the available data.
Since this is a Cochrane review, please note the following:
- Relative risk/odds ratios are used to establish significance, if you want to learn more about relative risk/odds ratios just click on the glossary link when the term comes up.
- The authors scour the Earth for any data on the subject and scrutinize every detail. Studies that don’t meet their high standards are not included.
- Studies that are included are combined and given a quality of evidence score:

Overall, the quality of the data is low to very low for these studies (39 studies in total).
Assisted hatching and live birth rate. No increase in live birth rate (30.1% with assisted hatching vs 28.3% without; odds ratio [95% CI]: 1.09 [0.92-1.29], based on 14 studies, low quality evidence).
Assisted hatching and live birth rate with ICSI or IVF. Increase in live birth rate (20.7% with assisted hatching vs 14.5% without), this was statistically significant (odds ratio [95% CI]: 1.54 [1.02-2.33]). Assisted hatching in IVF (no ICSI) showed no improvement in live birth rates.
Assisted hatching and live birth rate with different hatching methods. Chemical methods of assisted hatching, or with the laser method, showed no improvement compared to no hatching.
Assisted hatching and live birth rate in good or poor prognosis patients. Neither good nor poor prognosis patients had an improved live birth rate with assisted hatching. The poor prognosis group was close to being statistically significant but it wasn’t (29.4% with assisted hatching vs 22.7% without; odds ratio [95% CI]: 1.46 [0.99-2.15]). *Note that poor prognosis in this study refers to women with increased age, previous IVF failure, high FSH, or the study referred to the patient group as poor prognosis.
Assisted hatching and live birth rate with fresh or frozen embryo transfers. Performing a fresh or frozen transfer showed no improvement compared to no hatching.
Assisted hatching and chance of multiple pregnancy. Increase in the chance of multiples (12.1% with assisted hatching vs 9.1% without), this was statistically significant (odds ratio [95% CI]: 1.38 [1.13-1.68], based on 18 studies, low quality evidence).
Assisted hatching and chance of multiple pregnancy with ICSI or IVF cycles. The odds of multiples was higher when doing ICSI (3.09) than it was compared to IVF (1.87) – so doing ICSI with assisted hatching nearly doubled the odds of having multiples.
Assisted hatching and chance of multiple pregnancy in good or poor prognosis patients. The chance of multiples increased with poor prognosis (11.3% with assisted hatching vs 6.7% without, odds ratio [95% CI]: 1.95 [1.27-3.00]). There was no significant difference in good prognosis patients.
Assisted hatching and clinical pregnancy. Increase in the clinical pregnancy rate (36.3% with assisted hatching vs 32.2% without), this was statistically significant (odds ratio [95% CI]: 1.20 [1.09-1.33], based on 39 studies, low quality evidence).
Assisted hatching and clinical pregnancy in good or poor prognosis patients. Clinical pregnancy increased with poor prognosis (33.5% with assisted hatching vs 23.3% without, odds ratio [95% CI]: 1.68 [1.38-2.04]). There was no significant difference in good prognosis patients.
Assisted hatching and miscarriage rate. No impact on miscarriage rate (6% with assisted hatching vs 5.3% without), not statistically significant (odds ratio [95% CI]: 1.13 [0.82-1.56], based on 17 studies, very low quality evidence).
Zona thickening, or hardening, might explain why there are advantages for older/poor prognosis patients. In these patients, assisted hatching might help the embryo get out of the zona so it can implant. However, this study didn’t look at this detail.
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.









