A 2024 study compared outcomes of IVF cycles that transferred day 2/3 or day 5/6 embryos, finding that day 2/3 embryos have higher live birth rates per cycle, particularly for patients with 3 or less embryos.
What’s better? Day 3 embryo transfers or day 5? Does the embryo perform better in the uterus, or in the lab?
To address this, we can evaluate the success rates of complete IVF cycles that exclusively use either day 3 or day 5 embryo transfers. This is known as the cumulative live birth rate (CLBR), and is the aggregate of all the fresh and frozen transfers from a single cycle.
This post is a review of a study by Fauque et al. 2024, who compare the CLBR for cycles involving day 3 or day 5 embryo transfers. This study includes day 2/3 and day 5/6 (no day 7) embryos, but for simplicity I’ll just refer to them as day 3 or day 5 below.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Study details
This section covers key details of how the study was performed, including patient characteristics, how they were treated, and other methods used. For those who aren’t interested in these details, and just want to see the results, you can go ahead and skip this part.
- This study used data from the The Agency of Biomedicine, a national public institute in France that compiles medical data, and included data from 76 IVF centers in France between 2016 and 2019.
- The cycles included had to have at least one cleaved day 2 embryo. Exclusions: no egg donation, no women over 43, no PGT, no frozen eggs, no IVM, no day 1/4/7 transfers, no transfers with more than 3 embryos, no embryos frozen by slow freezing (ie. only vitrification).
- Cumulative live birth rate (CLBR) was defined as the delivery of at least one infant after 22 weeks, in either a fresh or frozen cycle (regardless of how many attempts were taken). Only the first delivery was considered, within a maximum of 2 years since the egg retrieval. After 2 years, nearly all of these cycles had used their frozen embryos in transfers. Patients could have done multiple IVF cycles (ovarian stimulations). The data I’m sharing here only looks at the 1 year follow up, with similar results to 2 years.
In terms of sample size, there were 133,250 egg retrieval cycles: 70,528 cycles with day 2/3 embryos and 62,722 cycles with day 5/6.
Due to the large sample size, there were differences in nearly all the patient characteristics. They performed multivariable logistic regression to control for female age, parity, number of embryos at day 2 (which was influenced by number of eggs retrieved and gonadotropin dose), method of fertilization, and the rank of IVF attempts.
This study includes day 2/3 and day 5/6 (no day 7) embryos, but for simplicity I’ll just refer to them as day 3 or day 5 below.
Explaining cumulative live birth rates per cycle and per transfer
When we’re talking about cumulative live birth rates (CLBR), we mean the overall chance of a live birth after having multiple transfers from a single IVF cycle. So if someone has an IVF cycle and gets 3 embryos, then has a fresh transfer followed by 2 frozen transfers, we’re considering the overall chance after these embryos are transferred.
This study considered both CLBR per embryo transfer and per cycle:
- CLBR per embryo transfer: This calculation includes the number of live births divided by the total number of embryo transfers (fresh and frozen).
- CLBR per cycle: This calculation includes the number of live births divided by the number of IVF cycles initiated (and includes all the transfers from the embryos produced from the IVF cycles). This rate also includes cycles where no embryos are transferred because of problems with embryo development or other reasons, and because of this CLBR per cycle is usually lower than CLBR per transfer.
For example, imagine 10 patients who have a total of 16 IVF cycles, with 12 transfers and 4 live births. The CLBR per transfer here will be 4/12 = 33%, and the CLBR per cycle will be 4/16 = 25%.
The important thing in this study is that day 3 embryos might arrest and stop developing before becoming blastocyst — so is it better to have a cycle where you go ahead and transfer day 3 embryos or wait for day 5? To address this, we want to look at the CLBR per cycle for day 3 vs day 5.
- If day 3 and day 5 CLBR per cycle are the same, then extended embryo culturing doesn’t have a negative impact on embryo development. In this case, culturing to day 5 would probably be preferred because there would be fewer transfer attempts (since some embryos arrest between day 3 and day 5).
- If the day 5 CLBR per cycle is higher than day 3, this suggests that extended culture actually increases embryo quality and the ability of embryos to lead to a live birth. Day 5 transfers should then be prioritized.
- If the day 3 CLBR is higher then this suggests that extended culture is decreasing embryo quality and that we’re missing out on some live births with day 5 transfers. This might be because some embryos are arresting with this extended culture, or becoming lower quality, so they’re not eligible for day 5 transfers. Day 3 transfers should then be prioritized.
The important thing to point out is that nothing is lost with day 3 transfers, but some embryos may arrest and not make it to day 5. Whether or not these embryos would have made it in the body isn’t clear, and is essentially the point of this study. There will likely be more transfers with day 3 vs day 5, and possibly more losses, but with unlimited time and resources, day 3 may be the better option.
CLBR per cycle is higher for day 3 transfers compared to day 5
Now let’s look at the results of the study! First we’ll look at the CLBR per cycle
Initially, they found that the CLBR per cycle for day 5 transfers appeared higher than it was for day 3 transfers (30.3% vs 33.4%, p< 0.0001). However, there were a lot of differences between these groups in terms of age, the number of IVF cycles performed, and other characteristics.
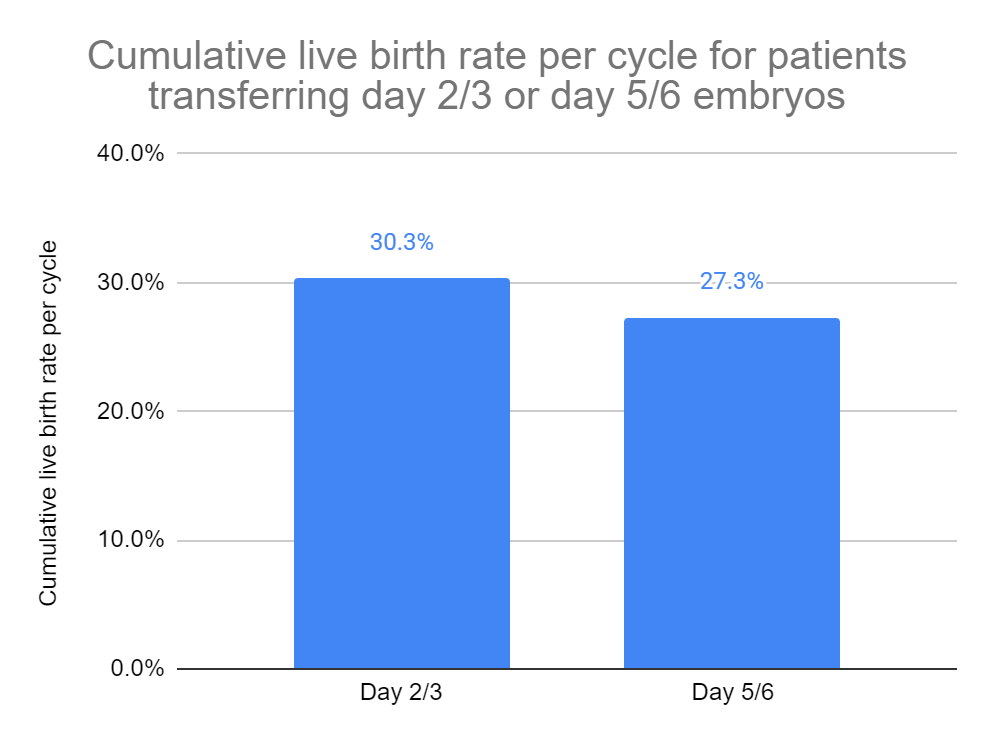
When they accounted for these differences in a statistical analysis, the results reversed: the CLBR per cycle was lower in day 5 transfers compared to day 3 (27.3% vs 30.3%; adjusted odds ratio [95% CI]: 0.84 [0.82-0.86]). This was after 1 year of follow up, when most of the embryos were transferred from a cycle. The results were similar after 2 years of follow up (when nearly all the frozen embryos were transferred).
I think CLBR can be a bit confusing to understand, so let’s break it down more to help make sense of it!
- In this study there were 133,250 egg retrieval cycles: 70,528 retrievals with day 3 embryo transfers and 62,722 retrievals with day 5 embryo transfers.
- Each egg retrieval cycle resulted in multiple embryos, which were transferred fresh or frozen. After 1 year, most of these embryos made from these 133,250 egg retrieval cycles were transferred.
- The study measured the chance of a live birth after transferring most embryos made from a single ovarian stimulation cycle, termed the CLBR per cycle.
- After adjusting for differences between groups, the CLBR per cycle showed that day 3 transfers had a higher live birth rate (30.3%) compared to day 5 transfers (27.3%). Of the 70,528 day 3 cycles, 21,370 (30.3%) of them resulted in a live birth (regardless of the number of transfers done in each cycle).
- In other words, women who opted to have day 3 transfers from a cycle were more likely to have a live birth compared to those who had day 5 transfers.
The increase in CLBR was 3% (30.3% vs 27.3%). This suggests that some day 3 embryos may have done better in the body compared to in the lab. However, the effect size of 3% is small, and likely resulted in more transfers than the day 5 group (see below). Also, they DID NOT include day 7 embryos in this study, so it’s possible that there wouldn’t even be a difference if these groups were included.
This study included 73 IVF clinics in France, including a wide range of patients and embryo qualities. When they redid the analysis and only included 23 of the top performing centers (with the highest CLBRs), they didn’t find a difference. One way clinics could boost their rates is by being selective with who they accept into their clinic, while also discarding poor quality embryos. So it’s possible (in my opinion) that if we only consider good prognosis patients and higher quality embryos, there may be no difference in per cycle outcomes.
CLBR per transfer is lower with day 2 or 3 compared to day 5 or 6
The data above is the CLBR per cycle, which tells us about how each ovarian stimulation cycle performed after most embryos were transferred fresh or frozen. What happens when we look at CLBR per transfer, and consider the number of actual transfer attempts made?
There was a higher rate of embryo transfer cancellation in the day 5 group compared to day 3 (19.9% vs 3.0%, p< 0.0001, excluding freeze-all cycles). This resulted in fewer transfers for day 5, which boosted the CLBR per transfer for day 5 vs day 3 (adjusted odds ratio [95% CI]: 1.12 [1.09-1.15], or a 12% increase). This is because there were fewer day 5 transfers, and when the CLBR is divided by a smaller number, the CLBR per transfer will be higher.
Patients with fewer embryos should transfer on day 3, not day 5
Next, the researchers wanted to see if day 3 or day 5 cycles were better in certain clinical situations. To do this, they followed CLBR per cycle for the groups over the course of a year. They reported this data based on the patients’ age, the number of (cleaved) embryos they had on day 2 (ie. more than one cell), and the number of IVF attempts they had.
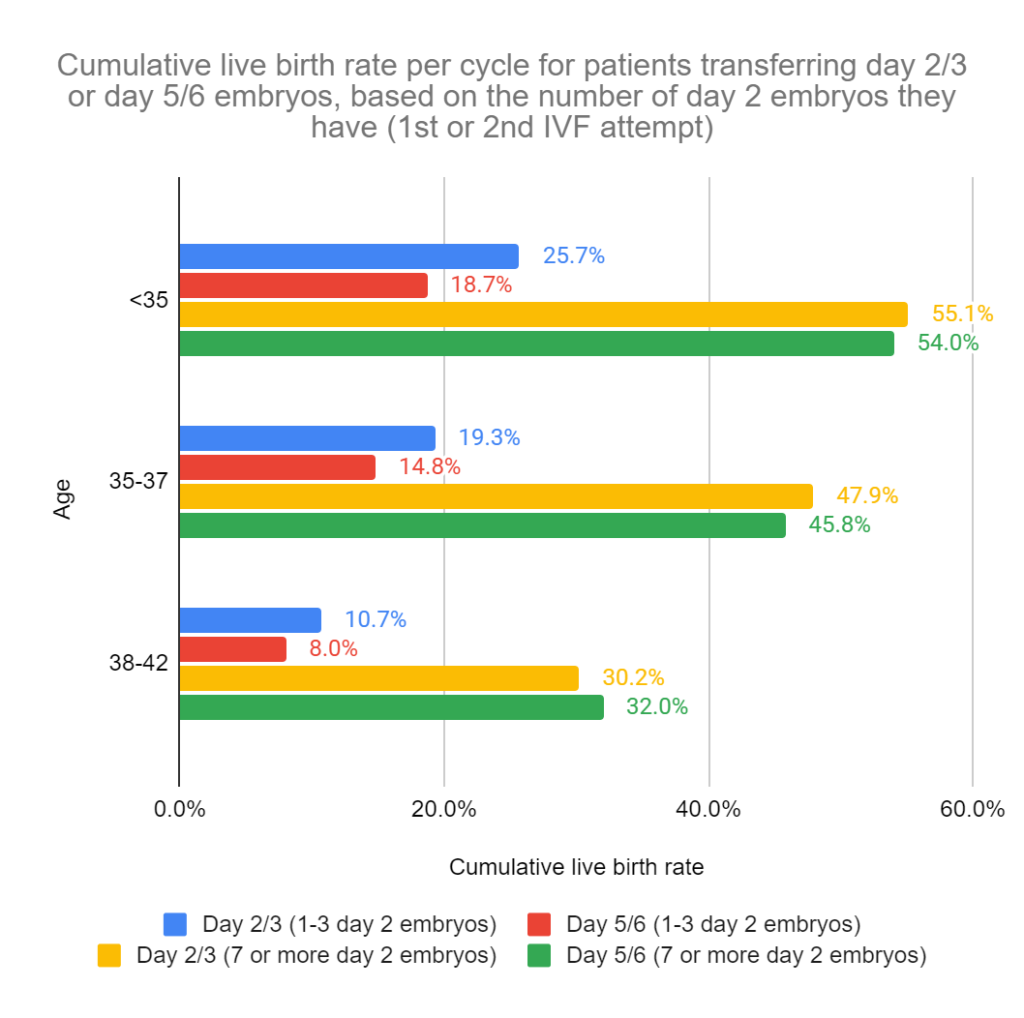
The first graph (below) shows data for patients based on their 1st or 2nd IVF attempt. They found that the CLBR was higher for day 3 groups vs day 5 when they had 1-3 embryos, regardless of age (the blue bar is longer than the red bar; this was statistically significant). There was no difference between the groups when they had 7 or more embryos.
Next, let’s look at the data for patients who had 3 or more IVF attempts. Again, they found that the CLBR was higher for day 3 groups vs day 5 when they had 1-3 embryos (which showed more of a difference compared to the previous graph), and there was no difference between the groups when they had 7 or more embryos.
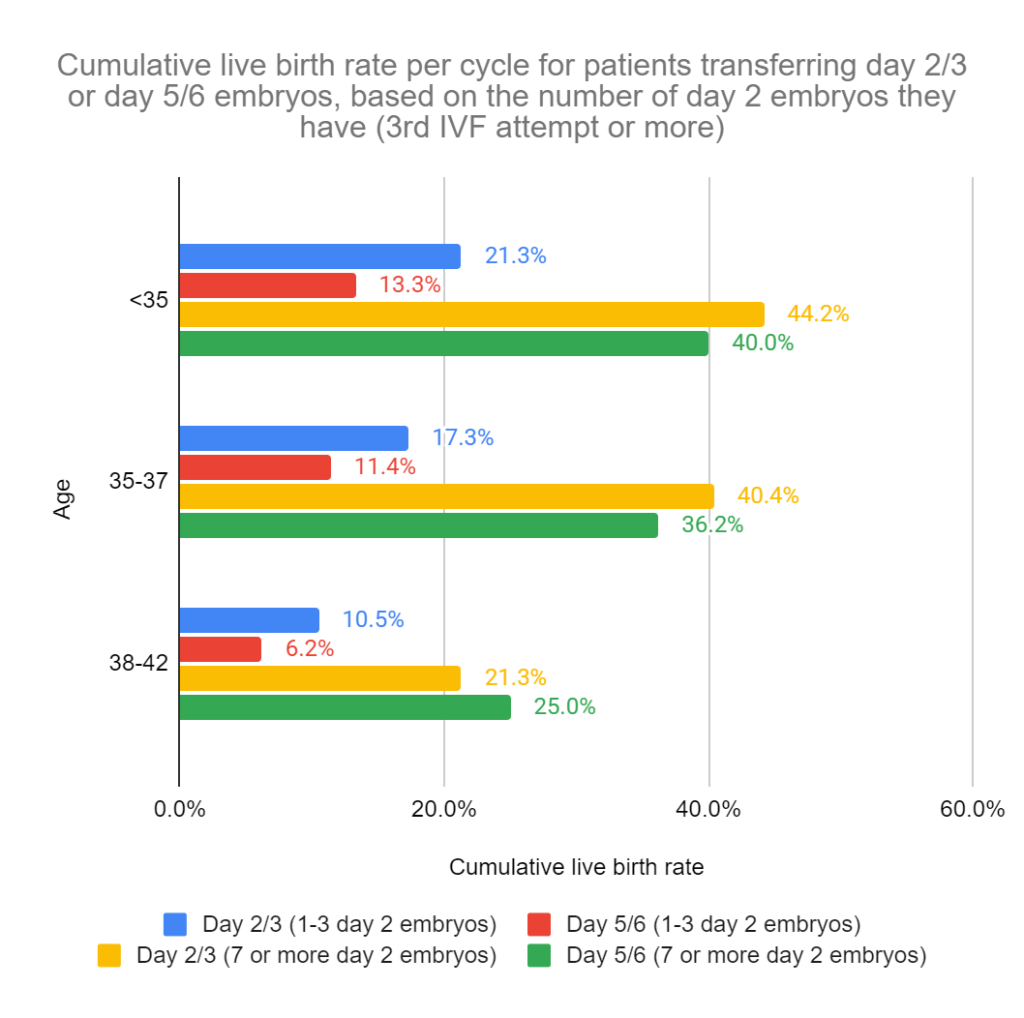
This tells us that patients with 1-3 cleaved embryos on day 2 should perform day 3 transfers instead of day 5 transfers, because there’s a higher chance of live birth (cumulatively, after most embryos have been transferred from the cycle). Patients with 7 or more should extend culture to day 5.
So what about those with 4-6 embryos on day 2? Unfortunately, they didn’t look at this, so it’s not clear. It might be best to split culture, and let the better quality embryos go to day 5 while the lower quality embryos are transferred or frozen on day 3 (lower quality embryos may not be able to tolerate the stress of extended culture as much as the better quality embryos). This is my opinion, and not the authors, and is something worth discussing with your doctor.
Conclusion
This study found that the CLBR per cycle was higher for the day 3 group compared to day 5, but only slightly. This suggests that some day 3 embryos may perform better in the body compared to in the lab.
There was a higher rate of embryo transfer cancellation in the day 5 group compared to day 3, which resulted in fewer transfers for day 5 that boosted the CLBR per transfer for day 5 vs day 3.
They also looked at day 3 vs day 5 in different clinical situations, and found that the CLBR was higher for day 3 compared to day 5 when patients had 1-3 embryos.
In other words, patients with 3 or fewer embryos should transfer on day 3 rather than extending culture to day 5. This was especially true for those with a history of 3 or more IVF cycles.
The authors note that it’s possible that culturing embryos to day 5 may be stressful for some embryos, resulting in embryo arrest or lower quality.
While this is a large study, other data on this subject has mostly shown no difference for CLBRs. These studies suggest that there’s no difference for day 3 vs day 5, and that day 5 transfers may be preferred since there would likely be fewer transfer attempts.
- A recent meta-analysis that combined multiple studies found better outcomes with blastocysts vs cleavage stage embryos on a per transfer basis, but not for the CLBR, although the quality of evidence was rated as very low. You can read more about this study in my post Meta-analysis compares cleavage stage (day 3) and blastocyst (day 5) transfer outcomes.
- Other studies (referenced below) have mainly found no difference in CLBR, although some look only at good prognosis patients (including a recent RCT), and only one has looked at outcomes for patients with few embryos like this study did (finding no difference in CLBR).
Related studies
To learn more about this topic, you can check out a number of studies referenced in this study below (6 links):
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.










