A 2025 study found that aging eggs and their support cells may have increased ribosome activity that contributes to reduced egg quality, and early clinical results suggest that rapamycin may help improve embryo quality and pregnancy rates.
As women age, their egg quality declines, leading to fewer embryos and lower pregnancy rates in IVF. While chromosomal errors are a leading cause for this, there may be additional factors that contribute to ovarian aging and reduced success rates.
A study by Li et al. (2025) examined one mechanism that hasn’t received much attention in reproductive medicine: how eggs manage the proteins they produce. Protein synthesis is controlled by the ribosome, a cellular machine that builds new proteins from the maternal RNA stored in the egg.
Proteins begin as simple chains and then must fold into the correct shape to function. If too many new proteins are produced at once, or if the egg’s quality-control systems slow with age, more of them misfold and become difficult to clear. This buildup of damaged proteins is a form of stress linked to cellular aging.
The research team wondered whether this imbalance also affects aging follicles, and whether rapamycin, a drug that slows ribosome activity, could improve outcomes for IVF patients.
The authors approached this question in two steps:
- First, they examined oocytes and cumulus cells from one group of IVF patients to look for age-related changes in ribosome activity. Cumulus cells surround the egg and help support its growth and maturation, so changes in these cells can influence the environment the egg develops in.
- Then they ran a randomized controlled trial to test whether short-term rapamycin could improve IVF outcomes in a different group of patients.
🔗 Original studies are referenced in this post or within the linked Remembryo posts.
💡 Reminder: Terms underlined with a dotted black line are linked to glossary entries. Clicking these does not count toward your paywall limit.
Aging follicles show increased ribosome activity and stress levels
The team analyzed oocytes and cumulus cells from 100 IVF patients aged 23–48 with normal ovarian reserve, using samples collected from GV-stage oocytes that would normally be discarded. They used these eggs to look for age-related molecular patterns.
- Oocytes showed a major gene expression shift around age 34. Older oocytes had more ribosome related genes turned on, while genes needed for meiosis and DNA repair were reduced.
- Cumulus cells showed even stronger age related changes. Their ability to clear damaged or misfolded proteins declined, oxidative stress genes dropped, and ribosome related genes increased with age.
- Signs of increased ribosome production appeared in multiple ways. For example, there was an increase in the levels of ribosomal RNA, the core building material for ribosomes.
Overall, this suggests that aging follicles may be making proteins faster than they can manage, leading to stress and reduced quality in both oocytes and cumulus cells. Using mice, they tested the drug rapamycin, a drug that can slow ribosome production and protein synthesis.
- Rapamycin improved several aging-related features in mice, including reducing excessive protein production signals, lowering oxidative stress and reducing the buildup of misfolded or aggregated proteins.
Taken together, the human and mouse results suggested that reducing protein production might improve the environment of aging oocytes. This set the stage for the next step: testing rapamycin directly in IVF patients through a randomized controlled trial.
Rapamycin improved IVF and pregnancy outcomes
Here’s the study details for the clinical trial, which used a separate group of patients from above:
- Study type: Non-blinded randomized controlled trial that took place at a single center in China in 2023.
- Participants: 100 infertile women with more than one prior failed IVF cycle, average age about 36 years with an AMH of about 1 ng/ml and AFC of 5. About 75% were under age 40, which is a limitation and doesn’t fully line up with the age-related molecular findings from above.
- Intervention: No treatment vs 1 mg oral rapamycin daily for ~21–28 days, started at pituitary downregulation and continued through ovarian stimulation until oocyte retrieval. 50 per group (randomized).
- Embryo transfer: High-quality embryos were transferred either on day 3 or day 5–6 based on embryo quality and patient preference.
- Primary outcomes: Number of oocytes and number of embryos.
- Trial registration: ChiCTR2300069828
Women who received rapamycin showed improvements in their IVF outcomes:
- Number of mature eggs retrieved: No difference — Median of 3 vs 2.
- Fertilized eggs: Higher — Median of 3 vs 2 in controls (p= 0.012).
- Number of day 3 embryos: Higher — Median of 2 vs 1 (p= 0.001).
- Number of blastocysts: Higher — Median of 2 vs 1 (p= 0.012).
- Number of top-quality blastocysts: Higher — Median of 1 vs 0 (p= 0.043)
They also compared clinical pregnancy rates after embryo transfer. Because the trial included both day 3 and day 5–6 transfers, they reported outcomes for each stage as well as the overall rate.
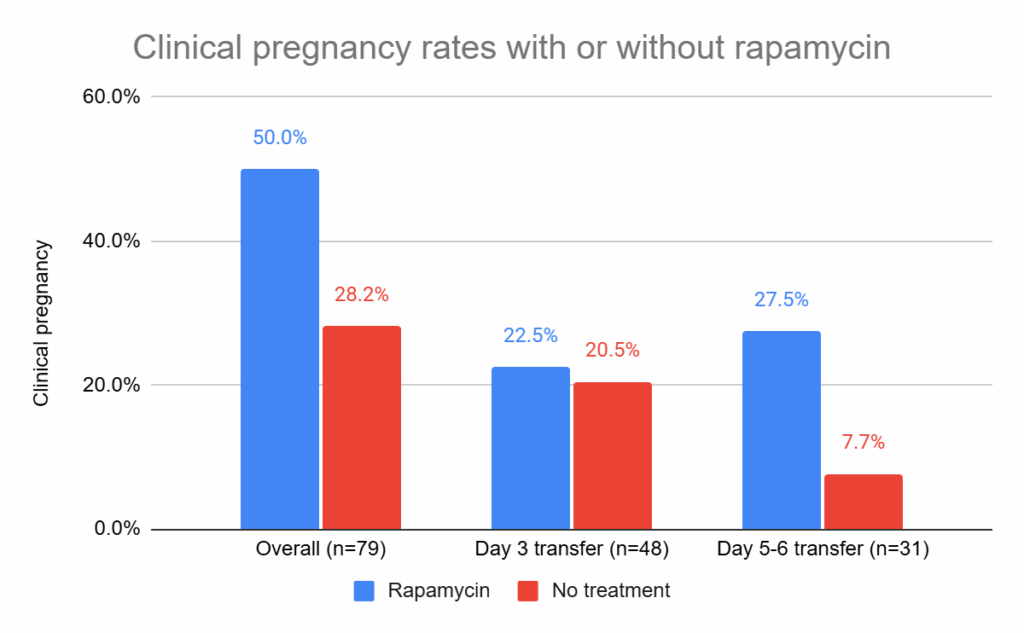
There was a statistically significant increase in the overall pregnancy rate (50.0% vs 28.2%, p= 0.047), and for day 5-6 (27.5% vs 7.7%, p= 0.021), but no difference in the day 3 group. This shows that the overall difference in pregnancy rates were attributed to blastocyst transfers. There were no statistical adjustments to control for age or other confounders.
Conclusions
This study found that older oocytes and cumulus cells showed signs of increased ribosome activity and reduced ability to respond to oxidative stress, with rapamycin partially reversing these effects in mice.
When testing this drug in humans, they found that rapamycin treatment resulted in an increase in the number of fertilized eggs, embryos and high quality blastocysts. There was no increase in the number of eggs retrieved.
Transfer of these embryos resulted in higher pregnancy rates overall, which was driven by patients who transferred blastocysts. There was no difference in day 3 transfer pregnancy rates.
The authors propose that as eggs and their surrounding cumulus cells age, ribosomes become overactive, leading to a buildup of defective proteins that can reduce egg quality. Rapamycin may restore balance by slowing down ribosome production to ultimately improve egg quality.
While encouraging, the clinical data are still preliminary and based on a small group of women. Importantly, most participants were under 40, which doesn’t really line up with the study’s idea of overactive ribosomes in older eggs.
The study registration (ChiCTR2300069828) listed its objective as evaluating rapamycin in women with diminished ovarian reserve, but the published paper did not require DOR or specific AMH/AFC levels. Although the average AMH and AFC were around 1 ng/ml and 5, these levels were not part of the inclusion criteria, so the true range of ovarian reserve in the group is unclear. Because most participants were also under 40, it’s not clear which patient population the trial was intended to target.
This isn’t the first study to explore rapamycin in IVF, but it’s one of the few to dig into possible molecular mechanisms. Larger trials are needed to confirm differences in pregnancy outcomes and to clearly report live birth rates, loss rates, and any safety concerns. Future studies also need to determine which patients benefit most.
Limitations. Unadjusted for confounders, mixed day 3 and 5-6 transfers, single center, and using GV-stage eggs for the lab work, which may not represent how mature, healthy eggs from older women behave. Additionally, the trial was powered to detect a 30% difference in pregnancy rates and did not reach that threshold, meaning it likely lacked enough participants to reliably detect differences.
Related studies
These are additional studies that haven’t been covered on Remembryo. They may be helpful if you’re exploring this topic further. This section is available for paid subscribers.
Reference
If you liked this post and want to support what I do, please consider a paid subscription, Patreon or donate through PayPal!

About Embryoman
Embryoman (Sean Lauber) is a former embryologist and the founder of Remembryo, an IVF research and fertility education website. After working in an IVF lab in the US, he returned to Canada and now focuses on making fertility research more accessible. He holds a Master’s in Immunology and launched Remembryo in 2018 to help patients and professionals make sense of IVF research. Sean shares weekly study updates on Facebook, Instagram, and Reddit regularly. He also answers questions on Reddit or in his private Facebook group.